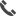Dr. Rice has joined Beacon Orthopedics and Sports Medicine
Congratulations Dr. Rice: 2025 Cincinnati Magazine Top Doctor
Labral Repair
Hip Scope Labral Repair
The acetabular labrum is a ring of strong fibrocartilaginous tissue lining around the socket of the hip joint. The labrum serves many functions where it acts as shock absorber, lubricates the joint, and distributes pressure equally along the weight-bearing surface. It also deepens the acetabular cavity and offers stability against femoral head translation.
A labral tear may be caused by trauma, femoroacetabular impingement (FAI), hip hypermobility, dysplasia, and degeneration. It is often associated with athletes playing sports as diverse as ice hockey, soccer, golf and ballet. Patients may have hip pain, clicking and locking of the joint and restricted range of motion. Patients may also experience dull pain on movement of the hip joint that may not subside on rest. Hip labral tear is often diagnosed with a comibination of clinical assessment (history and physical examination) and imaging studies (x-ray, MRI, CT).
First-line treatment for a hip labral tear typically consists of nonsurgical treatment including non-steroidal anti-inflammatory medication (NSAID), imaging-guided hip intraarticular injection, and physical therapy. In Dr. Rice’s practice population, success with nonsurgical treatment approaches 40-50%, although ranges in research studies vary broadly, as low as 20% and as high as 80+%. Because there is a chance of success with nonoperative treatment, it is attempted in most patients before considering surgery.
Surgical Treatment
If a patient fails nonsurgical treatment, and is an appropriate surgical candidate, then hip arthroscopy with labral repair may be the next step. This involves small portal incisions in the skin and specialized instruments to evaluate the joint with a camera. Using specialized tools, a labral tear can be identified and repaired with suture anchors. The anchors are non-metallic, and do not show on xray. The misshapen bone (FAI) is also corrected by shaving down the bumps with a small bone burr. The goal of labral repair surgery is to restore direct, stable contact between the acetabular rim and the labrum to encourage biologic healing, thereby resolving the patient’s pain and restoring function.
Frequently Asked Questions About Hip Labral Repair
What material are the suture anchors used for labral repair?
In Dr. Rice’s practice, labral repair is currently performed using 1.8mm all-suture anchors. These anchors are comprised entirely of suture material, with no metal or plastic retained in the patient, in contrast to some other products available on the market. The particular anchor used by Dr. Rice is among the smallest, most bone-conserving, and yet strongest of all hip labral anchors available today.
For hip labral repair, Is the suture material permanent or absorbable?
The sutures are made of permanent material (rather than absorbable), but in Dr. Rice’s anecdotal experience the suture material is synovialized, or enveloped, in fibrous healing tissue such that they virtually disappear from plain sight (as in the instance of followup arthroscopy). More importantly, there is no evidence the retained sutures cause any harm or damage to the hip cartilage or other structures.
How many suture anchors are needed to repair the labrum?
The number of suture anchors needed for labral repair varies based mostly on the size of the tear, while the pattern of tear, quality of tissue, and size of patient may also play a role, among other factors. 3-4 anchors is most common, but occasionally a tear will require only 1 or 2, and as many as 8 or 9. Functionally, the goal is to restore complete stability of the labrum to the acetabular rim.
How long does it take the hip labrum to heal back to the bone?
Similar to other soft-tissue-to-bone healing in the body, most believe the majority of labral healing occurs within 3-4 months after surgery. On the other hand, some studies indicate more subtle incremental healing occurs for at least 6 months after surgery, and improvements in patient function and symptoms may occur for 1-2 years after surgery.
What are the chances the hip labral repair will heal?
The chances of successful hip labral repair vary based on many factors including patient age, overall health, compliance with postop rehabilitation, and severity of the original labral tear/FAI, among others. For the purposes of guidance and helping patients develop reasonable expectations, Dr. Rice estimates approximately 80-90% of patients will heal appropriately and experience good to excellent functional outcomes after surgery. Perhaps 5-10% of patients will experience a failure of the labrum to heal or a re-tear of the labrum-patients in this group often have underlying risk factors to healing such as diabetes mellitus or a tobacco abuse history, or return to high-intensity, high-risk sport activities.
What are the advantages and disadvantages of hip labral repair versus hip labral debridement?
Advantages: Patients generally experience better functional outcomes from hip labral repair, particularly in long-term follow-up (10 years and beyond). It is believed by repairing the labrum its anatomic function is restored, and this is likely protective to the cartilage in the hip joint. Thereby, indirectly labral repair may help preserve the hip and protect against progression to degenerative osteoarthritis or the need for hip replacement. This theory is still being validated by high-quality clinical research, but most hip arthroscopists believe this to be a beneficial effect of labral repair.
Disadvantages: Hip labral repair is more technically demanding and consumes more operative time than simple debridement, which could be associated with a higher incidence of surgical complications. Labral repair is somewhat fragile in the early stages of postop healing, and therefore recovery is longer and slower than labral debridement.
What happens if my labral tear is not repairable?
In most cases, the torn labrum is repairable. In the case of a truly irreparable labral tear, generally two options are available: labral debridement, or labral reconstruction/augmentation. With the aim of restoring hip function and joint preservation, labral reconstruction/augmentation has become the preferred choice in most cases. Labral reconstruction utilizes graft tissue (typically semitendinosis allograft) to rebuild or reconstruct a new labrum, restoring the soft tissue bumper. Some studies have demonstrated the tendon graft tissue morphologically changes over time into more labrum-like tissue from a microscopic/histologic perspective. It is believed labral reconstruction will provide better long-term results for irreparable labral tear than labral debridement, but its widespread adoption has occurred relatively recently, and extensive long-term data on its efficacy is lacking. Regardless, labral reconstruction is one of the most exciting developments in hip arthroscopy in the past 5-10 years and provides another tool for hip arthroscopists to help patients with severe labral pathology.
If my labral tear is not repairable, will you reconstruct the labrum in the same surgery? Or is a second surgery required?
This scenario is routinely discussed in the office preoperatively, and a patient’s preference is noted, namely whether they prefer debridement of labral reconstruction in the event of a truly irreparable labral tear. Most patients defer to Dr. Rice’s judgment for this intraoperative decision, noting that Dr. Rice will act in the best long-term interest of the patient and his/her hip. Preoperative surgical consent will therefore typically include a plan for labral repair, but also included is “possible labral reconstruction/augmentation as indicated” or “surgery as indicated,” granting Dr. Rice the flexibility to perform the best surgery for a given patient. Therefore, in virtually all cases, labral reconstruction is performed at the time an irreparable tear is identified, and does not require a second surgery event.
Case Example #1
Intraoperative photo with suture passing device to repair hip labrum
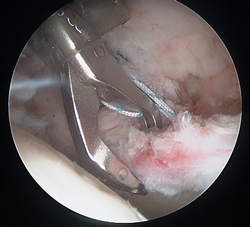
Completed 3-anchor hip labral repair with restoration of chondrolabral seal
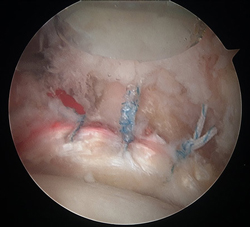
Case Example #2
Severely damaged and macerated labral tear in young athlete
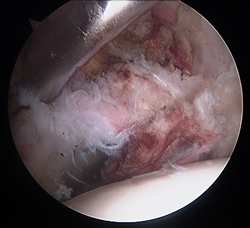
4-anchor labral repair complete
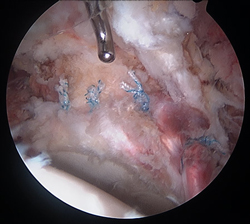
Case Example #3
33yo active female runner with 9 months of hip pain preventing sport activity. After 6 months of failed nonsurgical treatment, patient elected for hip arthroscopy with labral repair.
Completed 4-anchor hip labral repair
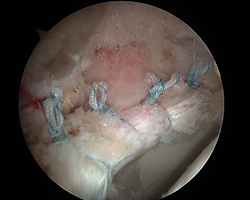
Patient returned to running and sport activity 6 months after surgery with no pain
nodisplay
nodisplay
Hip Procedures
- Hip Arthroscopy
- Labral Repair
- Acetabuloplasty (a.k.a. "Pincer takedown")
- Microfracture
- Femoroplasty (a.k.a. "CAM takedown")
- Synovectomy
- Ligamentum Teres Tear Debridement
- Iliopsoas Recession
- Subspine Impingement Decompression
- Endoscopic Abductor Tendon Repair
- Endoscopic ITB Release
- Endoscopic Bursectomy
- Proximal Hamstring Repair
- FAI FAQs
- Ischiofemoral Endoscopic Decompression