Dr. Rice has joined Beacon Orthopedics and Sports Medicine
Congratulations Dr. Rice: 2025 Cincinnati Magazine Top Doctor
Femoroacetabular Impingement
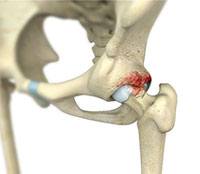
Femoroacetabular Impingement (FAI) refers to a process by which a misshapen hip joint experiences abnormal impingement throughout normal range of motion, gradually leading to breakdown in the joint. From a bony standpoint, the hip joint is comprised of the femur and the acetabulum, the name for the socket portion of the pelvis bone. The femoral head articulates with the acetabulum. In FAI, the femoral head/neck and acetabular socket abut or impinge on each other in an abnormal manner, and abut within an arc of motion when they should not touch. The damage can occur to the articular cartilage (the smooth white surface of the ball or socket) or the labral tissue (the lining of the edge of the socket) during normal movement of the hip. This breakdown of labrum and cartilage tissue causes pain and dysfunction, and left unaddressed may eventually lead to premature osteoarthritis. This process typically unfolds over months to years, but may be felt more suddenly.
FAI impingement generally occurs as two forms: Cam and Pincer.
CAM Impingement : The Cam form of impingement is when the femoral head and neck are not perfectly round, most commonly due to excess bone that has formed. This lack of roundness and excess bone causes abnormal contact between the surfaces.
PINCER Impingement : The Pincer form of impingement is when the socket or acetabulum rim has overgrown and is too deep. It covers too much of the femoral head resulting in the labral cartilage being pinched. The Pincer form of impingement may also be caused when the hip socket is abnormally angled backwards causing abnormal impact between the femoral head and the rim of the acetabulum.
Most diagnoses of FAI include a combination of the Cam and Pincer forms.
Symptoms of FAI
Symptoms of femoroacetabular impingement can include the following:
- Groin pain associated with hip activity
- Complaints of pain in the front, side or back of the hip
- Pain may be described as a dull ache or sharp pain
- Patients may complain of a locking, clicking, or catching sensation in the hip
- Pain often occurs to the inner hip or groin area after prolonged sitting or walking
- Difficulty walking uphill
- Restricted hip movement
- Low back pain
- Pain in the buttocks or outer thigh area
Risk Factors
A risk factor is something that is likely to increase a person’s chance of developing a disease or condition. Risk factors for developing femoroacetabular impingement may include the following:
- Athletes such as football players, weight lifters, and hockey players
- Heavy laborers
- Repetitive hip flexion
- Congenital hip dislocation
- Anatomical abnormalities of the femoral head or angle of the hip
- Legg-Calves-Perthes disease: a form of arthritis in children where blood supply to bone is impaired causing bone breakdown.
- Trauma to the hip
- Inflammatory arthritis
The cause of FAI is poorly understood. The best estimation of the etiology is genetic, meaning that it develops as a person grows into his/her adult skeleton, and was predetermined from their genetic makeup. It is known from research that FAI is more common among family members. Additionally, it is believed FAI may become exacerbated or worsened by certain types of repetitive activities, particularly high-flexion activity like sprinting or other running sports, deep squats and lunges, gymnastics, dance, and other activities. It is known, for example, that elite football players have a higher prevalence of CAM-type FAI. Repetitive stress injuries may cause reactive bone formation, the body’s attempt to reinforce the bone in response to stress, and grow a larger bump on the femoral neck or create a more prominent shelf on the acetabular socket. This may lead to a mild form of FAI becoming more severe over time.
Diagnosis
Hip conditions should be evaluated by an orthopaedic hip surgeon for proper diagnosis and treatment.
- Medical History
- Physical Examination
- Diagnostic studies including X-rays, MRI scans and CT Scan
Femoroacetabular Impingement is a disorder of misshapen bones around the hip, the femur and acetabulum. For that reason, FAI may be diagnosed with proper xrays. The views typically ordered to evaluate for FAI include an AP Pelvis, Frog-leg lateral, Cross-table lateral, and False Profile views. Other views, such as a Dunn view, can be substituted for the previously mentioned views.
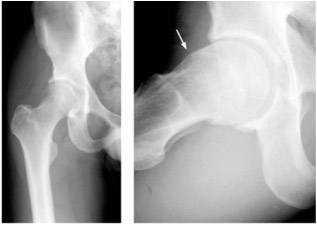
On an AP Pelvis view, numerous calculations are made to determine whether FAI is present. Two of the most important are center-edge angle and alpha angle:
Center-edge angle (CE angle) measures a vertical line from the center of the femoral head (measured as the center of a perfect circle) and another line connecting the center of the head to the lateral most edge of the acetabulum. The angle between these lines is the CE angle. A normal CE angle is 25-39 degrees. CE angle below 25 degrees suggests borderline, mild (<20), or moderate/severe (<15) dysplasia of the acetabulum (i.e. a socket that is too shallow). Hip arthroscopy for dysplastic hips can make patients worse by destabilizing a joint that already has inadequate bony stability due to the shallow socket. These patients are rarely a candidate for hip arthroscopy. CE angle >40 indicates a pincer lesion, in which the acetabular socket is excessively deep, and restraining normal hip range of motion. If the medial edge of the acetabulum crosses the ilioischial line, the condition is called acetabuli profunda, or deep socket. If the medial edge of the acetabulum crosses the iliopectineal line, this condition is called acetabula protrusio, or a protruding deep socket, and more severe condition. These patients have global, rather than focal, overcoverage of the socket, and are seldom a good candidate for hip arthroscopy unless there is only a focal area of their overcoverage responsible for problems.
To determine focal overcoverage, xrays are evaluated for a cross-over sign, in which the anterior and posterior walls of the acetabulum criss-cross on the xray. This indicates probable acetabular retroversion and focal overcoverage of the acetabulum, typically in the anterolateral portion of the acetabulum, in what is referred to as the 12 oclock to 3 oclock range of the socket. Another important sign of acetabular retroversion is an ischial spine sign, in which the normally hidden ischial spines are visible within the pelvic basin on xray.
Alpha angle is a measurement to discover Cam lesions of the femoral neck. A perfect circle is made around the femoral head, and an angle is formed with a line bisecting the femoral neck to the center of the head, and another line connecting the center with the point along the head in which the bone deviates from the perfect circle. The larger the bump on the femoral neck, the sooner it breaks from the perfect circle, and the larger the angle. Normal alpha angle may be debated, with most experts agreeing between 50-55 degrees. An alpha angle above 55 degrees is usually a sign of a Cam lesion.
The lateral edge of the femoral neck on an AP Pelvis correlates with the 12 oclock position on the femoral neck clockface, in which the femoral neck is conceptualized in an axial plane to understand its three-dimensional structure. To assess for a Cam lesion at other positions of the clock face, the Frog-leg (2:00) and cross-table (3:00) views are obtained. This provides a more comprehensive assessment of the area of the femoral neck (12-3:00) where Cam lesions most commonly occur.
The acetabular false profile view provides valuable information about the joint space, and the anterior center edge angle. Often times a hip joint will appear healthy, with normal joint space, and there is no clear evidence of degenerative disease or arthritis. Because the anterolateral portion of the joint is often the first to reveal subtle joint space narrowing (and early arthritis), this view can help identify hips with early arthritic changes that are less likely to benefit from hip arthroscopy. Also, anterior center edge angle (anterior CE) less than 20 degrees may be a sign of anterior bony undercoverage and risk of instability or micro instability after surgery.
Occasionally CT scan, often with 3-dimensional reconstructions, is necessary to fully appreciate and understand the shape and morphology of the deformity. This is often performed after a decision has been made to proceed with arthroscopic FAI correction to help guide the surgeon in bony resection.
MRI
FAQ: What is the next step in imaging after initial xrays? How do I evaluate the status of my cartilage, labrum, and other soft tissues?
Answer:If a patient has FAI and pain the in the hip, with concern for labral tear based on exam, an MRI arthrogram may be indicated to confirm the diagnosis and evaluate the soft tissue structures that can not be visualized with xray. An arthrogram involves injected dye into the joint to assist in detecting the tear. This increases the sensitivity of the test for detecting the tear. MRI Athrogram is capable of detecting labral tear, cartilage damage, presence of cysts, such as degenerative subchondral cysts, as well as extraarticular (outside the hip joint) problems such as muscle tears or strains and tendinosis/tendinopahty (breakdown of the tendon), and in athletes especially can evaluate the bone for stress fracture and other bony pathology. The MRI can not only detect the damage present in the hip, but help the hip orthopedic surgeon determine whether the pathology can be successfully addressed with hip arthroscopy.
FAQ: I already obtained an MRI of my hip from another physician. Why do I need another MRI?
Answer: There may be several reasons an MRI must be repeated in the workup of a hip problem and possible labral tear. First, MRI Arthrogram is typically the gold standard of diagnosis in hip labral tears, and plain MRI may not provide sufficient clarity to determine whether a labral tear is present versus a naturally occuring variant of normal anatomy, such as a cleft. Secondly, because FAI and labral tears involve complex, intricate anatomy deep in the joint, a high quality, high resolution image is necessary for accurate diagnosis and proper decision making. If a poor quality MRI was performed intially, as determined by the orthopedic surgeon, another MRI Arthrogram in a high quality scanner will be needed. Finally, if the MRI was performed at least one year prior, or a significant new injury has occurred since the original MRI, a new MRI will most likely be needed. As in all cases, Dr. Rice reviews all cases on an individual basis to make the best decision for each patient.
Treatment Options
Conservative treatment options refer to management of the problem without surgery. Nonsurgical management of FAI will probably not change the underlying abnormal biomechanics of the hip causing the FAI but may offer pain relief and improved mobility.
Conservative Treatment Measures
- Rest
- Activity Modification and Limitations
- Anti-inflammatory Medications
- Physical Therapy
- Injection of steroid and analgesic into the hip joint
The first line of treatment involves nonsurgical treatment including physical therapy, oral anti-inflammatory medication, activity modification (avoiding painful activities), and a hip corticosteroid injection. This is usually achieved in the office under ultrasound guidance.
Surgical Treatment
Hip arthroscopy to repair femoroacetabular impingement is indicated when conservative treatment measures fail to provide relief to the patient.
If a patient fails nonsurgical treatment, and is an appropriate surgical candidate, then hip arthroscopy may be the next step. This involves small portal incisions in the skin and specialized instruments to evaluate the joint with a camera. Using specialized tools a labral tear can be identified and repaired with anchors and sutures. The anchors are non-metallic, and do not show on xray. The misshapen bone (FAI) is also corrected by shaving down the bumps with a small bone bur. Xray is utilized during the procedure to provide real-time feedback during the sculpting process.