Dr. Rice has joined Beacon Orthopedics and Sports Medicine
Congratulations Dr. Rice: 2024 Cincinnati Magazine Top Doctor
Hip Arthroscopy
Hip Scope Labral Repair
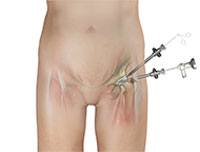
Arthroscopy, also referred to as minimally invasive surgery, is a procedure in which an arthroscope is inserted into a joint to check for any damage and repair it simultaneously.
An arthroscope is a small, fiber-optic instrument consisting of a lens, light source, and video camera. The camera projects an image of the inside of the joint onto a large screen monitor allowing the surgeon to look for any damage, assess the type of injury, and repair the problem.
Hip arthroscopy is a surgical procedure performed through very small incisions to diagnose and treat various hip conditions including:
- Removal of torn cartilage or bone chips that cause hip pain and immobility.
- Repair a torn labrum: The labrum is a fibrous cartilage ring which lines the acetabular socket.
- Removal of bone spurs or extra bone growths caused by injury or underlying misshapen hip, formally known as femoracetabular impingement.
- Removal of part of the inflamed synovium (lining of the joint) in patients with synovitis. This procedure is called a partial synovectomy.
- Evaluation and diagnosis of conditions with unexplained pain, swelling, or stiffness in the hip that does not respond to conservative treatment.
Hip arthroscopy is performed under regional or general anesthesia depending on you and your surgeon’s preference. Often a regional nerve block such as a fascia iliacus block is offered to reduce postoperative pain in the first 12-24 hours after surgery. The anesthesiologist will help you decide by reviewing the potential risks and benefits of the nerve block procedure.
Surgery typically includes 3 or 4 small incisions about 1/4 inch in length around the hip joint, anterior and lateral. Through one of the incisions an arthroscope is inserted. Along with it, a sterile saline solution is pumped into the joint to expand the joint area and create room for the surgeon to work.
The larger image on the television monitor allows the surgeon to visualize the joint directly to determine the extent of damage so that it can be surgically treated.
Surgical instruments will be inserted through other tiny incisions to treat the problem. Common devices used include a shaver, radio-frequency ablation device, small scalpel, suture and tissue graspers, drill guides, cannulas, etc.
After the surgery, the incisions are closed and covered with a bandage. Watery drainage from the portal sites is expected after surgery, as this represents egress of the saline solution pumped into the joint throughout the procedure. Drainage decreases significantly after 48-72 hours.
The advantages of hip arthroscopy over the traditional open hip surgery includes:
- Smaller incisions
- Minimal trauma to surrounding ligaments, muscles, and tissues
- Less pain
- No need for implanted metal hardware
- No need for a bone osteotomy to heal (often required for open surgery access)
- Lower infection rate
- Less scarring
- Earlier mobilization
- Shorter stay (outpatient rather than inpatient surgery)
As with any surgery, there are potential risks and complications involved. It is very important that you are informed of these risks before you decide to proceed with hip arthroscopy surgery. Possible risks and complications include:
- Infection at the surgical incision site or in the joint space
- Nerve damage which may cause numbness, tingling, pain, and weakness; this occurs most commonly in the front of the thigh, although it may occur in the perineal region and genital region (pudendal nerve), or posterior thigh and leg (sciatic nerve). Areas of numbness and tingling are often temporary and spontaneously resolve within days or weeks, with rare cases lasting months. The area tends to gradually shrink over time and decrease in intensity. When this occurs, it most often affects only sensory function (ability to feel), and not the motor function (strength) of thigh or leg muscles.
- Excess bleeding into the joint, a condition called hemarthrosis
- Blood clots may form inside the deep veins of the legs which can travel to the lungs (pulmonary embolism). Aspirin is routinely provided for 4 weeks after surgery to prevent this complication
- Heterotopic ossification, or the formation of bone in the soft tissue. This is typically asymptomatic, but can become symptomatic if large. Naprosyn is provided for 3 weeks after surgery to prevent this complication.
- Femoral neck fracture is a rare yet catastrophic complication that may occur after femoroplasty to resect the CAM lesion in cases of femoroacetabular impingement. The underlying cancellous (honeycomb) bone is weaker than the normal cortical bone, creating a weak point in the femoral neck. This remodels and regains full strength during the recovery process. This is a major reason weight bearing is restricted for the first 4-8 weeks after surgery with crutches
- Re-tear of the labrum. While rare, future injuries may cause failure of the repair or re-tear in a new area of the labrum
- Need for future surgery, including the need for hip replacement surgery in the future. Often patients presenting with FAI and/or labral tear have sustained some level of cartilage damage or wear, and in most circumstances this damage is irreversible. Therefore, while a secondary goal of hip arthroscopy (primary goal is pain relief and functional improvement in present day) is to hopefully preserve the joint for years to come, damage existing prior to surgery may predict the need for further surgery in the future. For instance, some research indicates the risk of conversion to hip replacement within 2 years of hip arthroscopy varies by age: 3% risk under age 40, 16% risk ages 40-49, 26% risk ages 50-59, and 35% risk ages 60 and older.
Patients are advised to take certain precautions to promote faster recovery and prevent further complications. These include:
- Taking medications as prescribed.
- Use of crutches to prevent or limit bearing weight on the operated hip; most commonly 4-8 weeks after surgery with 50% weight bearing
- Physical therapy exercises should be performed to restore normal hip function and improve flexibility and strength
- Eating a healthy diet and avoiding smoking will help in faster healing and recovery; diabetic patients should maintain excellent glucose control
- Avoid activity which involves lifting heavy things or strenuous exercises for first few weeks after surgery
With advances in surgical techniques, arthroscopy plays an important role in diagnosis and treatment of hip diseases. Please schedule an appointment with Dr. Rice for a personalized consultation to determine if hip arthroscopy is the right choice for you.
nodisplay
nodisplay
Hip Procedures
- Hip Arthroscopy
- Labral Repair
- Acetabuloplasty (a.k.a. "Pincer takedown")
- Microfracture
- Femoroplasty (a.k.a. "CAM takedown")
- Synovectomy
- Ligamentum Teres Tear Debridement
- Iliopsoas Recession
- Subspine Impingement Decompression
- Endoscopic Abductor Tendon Repair
- Endoscopic ITB Release
- Endoscopic Bursectomy
- Proximal Hamstring Repair
- FAI FAQs
- Ischiofemoral Endoscopic Decompression